Hemolysis
Hemolysis is the breakdown of red blood cells accompanied by the release of the blood pigment — hemoglobin. The breakdown of erythrocytes can be:
- in the blood vessels (intravascular),
- outside the blood vessels (extravascular).
Hemolysis:
Hemolysis 2:
Physiologically, erythrocytes are damaged or too old (the normal lifespan of an erythrocyte is about 120 days[1]) and are taken up by the macrophages of the RES (reticuloendothelial system) of the liver, spleen and bone marrow, so it is extravascular hemolysis. Hemoglobin here breaks down into:
- globin – protein chains (two α and two β) that are used for the resynthesis of hemoglobin,
- biliverdin – a green linear tetrapyrrole, it is reduced to yellow bilirubin , which is bound to albumins and transferred to the liver, where it is conjugated with glucuronic acid and then excreted into the bile,
- Fe3+ – binds to apoferritin to form ferritin (a protein in the shape of a hollow sphere, in the cavity of which iron is stored in the form of Fe(OH)3 a FePO4), with an excess of iron above apoferritin, Fe is stored in the form of hemosiderin (a complex of hydrated Fe2O3 with proteins, polysaccharides and lipids) inside macrophages (siderophages).
Distribution of hemolysis by cause[edit | edit source]
- Osmotic hemolysis can occur in both hypertonic and hypotonic solutions. In a hypertonic solution, cells release water to the environment and shrivel, which can cause defects in the cell membrane. In a hypotonic solution, on the other hand, the cell fills with water, takes on a spherical shape and can burst (plasmoptysis).
- Physical hemolysis usually consists of mechanical damage to the membrane. We can cause it, for example, by shaking, but also by extreme temperature changes or ultrasound.
- Chemical hemolysis is mainly based on the chemical reaction of lipids in the membrane with a certain substance. Damage can be caused by strong acids or bases, surfactants, or fat solvents.
- Toxic hemolysis occurs under the action of some bacterial toxins. It can also be a reaction to the presence of animal (snake) or plant poisons.
- Immunologic hemolysis is typical when an incompatible transfusion is given. Complement is responsible for this reaction.
Extravascular hemolysis[edit | edit source]
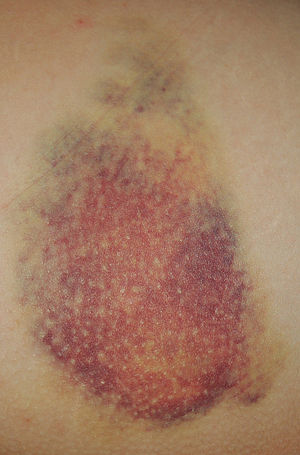
Outside the blood vessels, erythrocytes break down rapidly. Hemoglobin released from them (or whole erythrocytes) is phagocytosed by tissue macrophages and the resulting bilirubin diffuses into the surroundings and conditions the coloring of the surrounding tissues ( local icterus – typically in a subcutaneous hematoma, bruise). The icteric coloration later disappears and the rusty coloration persists (hemosiderin – e.g. in cerebral areas of hemorrhage). Another pigment that is created in this process is ceroid – a lipopigment arising from the polymerization of lipid oxidation products (lipids released from decayed erythrocytes), the mixture of ceroid and hemosiderin is called hemofuscin. Subsequently, the organization of the hematoma occursnon-specific granulation tissue – siderophages and fibrin are present on the periphery, along which granulation tissue grows into the hematoma, which penetrates it and only a small scar remains from the hematoma. If the hematoma is larger, then the central part can liquefy before the fibrin fibers have been replaced by granulation tissue, the surface layer of the hematoma acquires the properties of a semi-permeable membrane, through which fluid is sucked into the hematoma and the hematoma enlarges, forming a post-hemorrhagic pseudocysts, or after the discoloration of the posthemorrhagic hygroma.
Accelerated extravascular hemolysis is accompanied, for example, by hypersplenism, some disorders of erythrocyte metabolism, malaria, etc. The level of unconjugated bilirubin may be elevated (above 12 μmol/l), subicterus or icterus may be clinically evident. There are symptoms of hemolytic anemia - increased amount of reticulocytes, hemoglobinuria, anemia (hemoglobin below 120 g/l), reduced number of erythrocytes in the blood count, increased activity of lactate dehydrogenase.
Intravascular hemolysis[edit | edit source]
The breakdown of blood cells in the blood vessels can be caused by:
- erythrocytes themselves (corpuscular hemolysis),
- action of external factors (extracorpuscular hemolysis).
Hemoglobin released from disintegrating erythrocytes binds to haptoglobin, forming a complex that does not pass through the glomerular filter (the function of haptoglobin formed in the liver is to prevent both kidney damage and iron loss). The complex is phagocytosed by macrophages – hemoglobin breaks down, bilirubin and ferritin or hemosiderin are produced. With increased hemolysis, icterus and hemosiderosis occur . If the released hemoglobin is more than haptoglobin can bind (especially in acute hemolysis, the concentration of haptoglobin in the serum is reduced by consumption (norm 0.3-2 g/l)), hemoglobinemia occurs and the excess hemoglobin passes through the glomerular filter into the renal tubules - hemoglobinuria and hemosiderinuria occur(part of the hemoglobin molecules is taken up by the cells of the proximal tubule and converted into hemosiderin, which is then gradually released into the urine) - the precipitation of hemoglobin then causes kidney damage known as hemoglobinuric nephrosis (a similar impairment occurs in crush syndrome - myoglobinuric nephrosis).
Diagnosis of possible causes of hemolysis[edit | edit source]
Coombs test[edit | edit source]
is the detection of antibodies against erythrocyte surface antigens. Antiglobulin serum is added to the patient's washed erythrocytes, agglutination indicates the presence of immunoglobulins or complement components bound to the erythrocytes;
- direct Coombs test (also direct antiglobulin test) – enables the detection of red blood cells sensitized/coated with immunoglobulin and complement components "in vivo";
- indirect Coombs test - enables the detection of anti-erythrocyte antibodies present in the patient's serum or plasma - is important for people who are repeatedly given transfusions or erythrocyte concentrates.
Osmotic resistance tests[edit | edit source]
Using these tests, we examine the resistance of blood cells to low osmotic pressure in the environment (so-called minimum osmotic resistance, so-called maximum osmotic resistance),
- normal values average 0.4% NaCl for minimal and 0.3% NaCl for maximal osmotic resistance.
Enzymatic examination of erythrocytes[edit | edit source]
In the absence of glucose-6-phosphate dehydrogenase, there is insufficient formation of NADPH and thus reduced regeneration of glutathione. Erythrocytes (especially their membrane) are then susceptible to damage by reactive oxygen species.
Ham test[edit | edit source]
is a diagnostic (screening) test for paroxysmal nocturnal hemoglobinuria (PNH). Erythrocytes are incubated in serum acidified to pH 6.2, the acidic environment activates complement and pathological erythrocytes undergo hemolysis.
Flow cytometry[edit | edit source]
In this method, proteins bound to the cell membrane, which are involved in
- protection against the lytic effects of complement,
- the 2 proteins (MIRL and DAF) are designated by the antibodies that specifically react with them, CD-55 and CD-59.
References[edit | edit source]
Related articles[edit | edit source]
Source[edit | edit source]
- KITTNAR, Otomar, et al. Lékařská fyziologie. 1. edition. Praha : Grada, 2011. pp. 790. ISBN 978-80-247-3068-4.
- TROJAN, Stanislav – TROJAN, Stanislav, et al. Lékařská fyziologie. 4. edition. Praha : Grada, 2003. pp. 772. ISBN 80-247-0512-5.
References[edit | edit source]
- ↑ KITTNAR, Otomar – ET AL.,. Lékařská fyziologie. 1. edition. Praha : Grada, 2011. 790 pp. pp. 130. ISBN 978-80-247-3068-4.