Diuretics
Diuretics are drugs that act directly on the kidneys. They increase diuresis, affect Na + transport, inhibit NaCl reuptake and tubule water.
Thiazide diuretics:
Mechanism of action diuretics are associated with membrane transport. Diuretics may affect this transport in different parts of the nephron. They can also inhibit some transporters outside the kidneys. Their effect in the kidneys is most pronounced due to the highest concentration of these transporters.
Indications for diuretics
- Edema – the excretion of Na + and water will increase. The plasma volume decreases, the protein concentration in the blood increases, and thus the oncotic pressure, which draws extravascular fluid into the blood and reduces swelling;
- hypertension – reducing peripheral vascular resistance, thereby reducing pressure; heart failure – reducing peripheral resistance will make the heart easier, increase cardiac output and improve myocardial performance;
- prevention of renal insufficiency and decreased liver function – due to bleeding, there is a risk of circulatory failure, liver and urinary arrest.
Distribution of diuretics
- Acting in the proximal tubule (proximal diuretics)
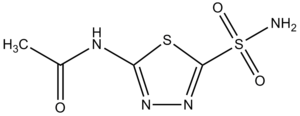
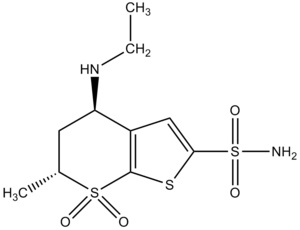
- Carbonic anhydrase inhibitors: acetazolamide, dorzolamide.
- Acting in the distal tubule (distal diuretics)
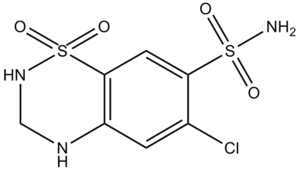
- Thiazides: hydrochlorothiazide, chlorthalidone.
- Acting in Henle's loop (loop diuretics)
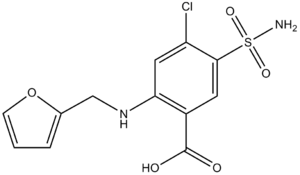
- Henle loop diuretics: furosemide, ethacrynic acid, muzolimine, etozoline.
- Saving potassium excretion
- Potassium-sparing: spironolactone, amiloride, triamterene.
- Increasing water excretion
- Osmotic diuretics: mannitol.
- Combination: hydrochlorothiazide + amiloride, chlorthalidone + amiloride.
- New: ADH antagonists.
Diuretics acting in the proximal tubule
This group of diuretics includes carbonic anhydrase inhibitors, which inhibit bicarbonate reabsorption in the proximal tubule with subsequent bicarbonate diuresis. Significant bicarbonate losses can lead to metabolic acidosis. However, the effect gradually decreases over several days. The cause is increased NaCl reabsorption, which leads to acidosis.
Representatives
The two main representatives are:
- Acetazolamid,
- Dorzolamid.
Indications
The main indication is glaucoma therapy. The ciliary body secretes bicarbonate into the intraocular fluid by a mechanism similar to tubular reabsorption, but in the opposite direction. It can also be blocked by carbonic anhydrase inhibitors, leading to a decrease in the amount of intraocular fluid. Dorzolamide is given as eye drops. Another indication is the correction of metabolic alkalosis and prophylaxis and treatment of altitude sickness.
Side effects and toxicity
- Metabolic acidosis.
- Kidney stones - Phosphaturia and hypercalciuria develop during bicarbonate diuresis. Under these conditions, calcium salts become potentially insoluble at alkaline pH, thus meeting the conditions for stone formation.
- Hypokalaemia.
- CNS disorders - confusion, drowsiness.
Loop diuretics
Loop diuretics act by blocking Na + transport in the ascending part of Henle's loop. This disrupts the osmotic stratification of the kidney and significantly increases diuresis. Compensatory mechanisms in the distal tubule and collecting duct lead to the exchange of Na + for K +, which can lead to severe hypokalaemia. It is therefore necessary to monitor the level of potassium, or increase its intake by infusion of KCl, or combine loop diuretics with potassium-sparing. With K + ions, Cl− ions are also lost, which can cause hypokalemic, hypochloremic metabolic alkalosis. At the same time, tubular resorption of Ca2 + and Mg2 + also decreases.
Representatives
Furosemide is one of the most commonly used.
Effects and uses
- Its vasodilating effect reduces preload.
- When administered intravenously, the onset of action is rapid (within 10 minutes) and lasts for 2-3 hours.
- It is used in acute conditions: hypertensive crisis, pulmonary edema, congestive heart failure, hypercalcemia.
Side effects
- Water and ion balance disorders,
- hypovolaemia, haemoconcentration to dehydration and hypotension,
- hyperuricaemia, GIT disorders, rash, hematopoietic disorders,
- increases the toxicity of cardiac glycosides.
Diuretics acting in the distal tubule
Here we rank mainly thiazide diuretics (thiazides), for which we distinguish:
- Renal effect: thiazides inhibit NaCl reabsorption by distal tubule epithelial cells into the blood. At the same time, they increase Ca2+ reabsorption in the distal tubule;
- Extrarenal effect: vasodilation in the postcapillary bed reduces the return of blood to the heart and consequently cardiac output. Vascular resistance decreases after 2-3 weeks.
Representatives
The main representatives are:
- Hydrochlorothiazide,
- Chlorthalidone.
Other representatives include: chlorothiazide, trichloromethiazide, bendroflumethiazide, methipamide, indapamide.
Indications
- Arterial hypertension;
- Heart Failure;
- nephrolithiasis caused by idiopathic hypercalciuria;
- diabetes insipidus- reduce the volume of urine in patients.
Contraindications
- decreased kidney function;
- pregnancy;
- dna;
- hypercalcemia.
Side effects and toxicity
- Hypokalaemic metabolic alkalosis and hyperuricaemia.
- Decreased glucose tolerance. Hyperglycemia may occur in diabetics and individuals with abnormal glucose test results. It is caused by a reduction in the release of insulin from the pancreas.
- Hyperlipidemia. Thiazides lead to approximately 5-15% increases in cholesterol and lipoproteins (LDL) in the blood. Due to long-term administration, these values may normalize.
- Dilution hyponatremia. This is a serious side effect. It is the result of increased ADH production due to hypovolemia, decreased renal dilution capacity and thirst. It can be prevented by reducing the dose of the diuretic or reducing water intake.
- Allergic reactions.
Potassium saving diuretics
Potassium-sparing diuretics act as aldosterone antagonists in the collecting duct and lower distal tubule. It can be a direct antagonism - for example, spironolactone acts as a blocker of the mineralocorticoid receptor. In contrast, for example, amiloride inhibits Na + transport by ion channels in the luminal membrane, thus reducing sodium resorption. This also reduces the loss of potassium into the urine, as the resorption of Na + from the collecting ducts creates a negative electrical potential in their lumen, which facilitates the secretion of K + and H + into the urine.
Representatives
The main representatives include:
- spironolactone: potassium canrenoate (active metabolite)
- amiloride
Indication
Increased mineralocorticoid effect due to primary or secondary aldosteronism. Secondary aldosteronism is due to heart failure, liver cirrhosis, nephrotic syndrome, and thiazide and loop diuretics.
Side effects and toxicity
- Hyperkalaemia can also be life-threatening. The risk of this complication is exacerbated when the kidneys are affected or when medicines (beta-blockers, non-steroidal anti-inflammatory drugs or ACE inhibitors) are given.
- Hyperchloremic metabolic acidosis can be induced by inhibition of H + secretion with concomitant K + secretion.
- Gynecomastia - spironolactone.
Osmotic diuretics
Osmotic diuretics are drugs that increase the excretion of water (diuresis). The proximal tubule and the descending limb of the loop of Henle are freely permeable to water. In these segments, the osmotically active osmotic diuretics, which are not reabsorbed, lead to water retention in the nephron. As a result, these substances lead to osmotic diuresis.
Examples
The main example of an osmotic diuretic is mannitol, which is administered as a 10-20% solution.
Mannitol is not metabolized and undergoes glomerular filtration (within 30-60 min after administration) without significant tubular secretion or reabsorption. Since mannitol is poorly absorbed in the GIT, per os administration is avoided. If performed, it would cause severe diarrhea. Hence, mannitol is usually administered intravenously. Due to osmotic diuretic administration, accelerated tubular fluid flow (and hence less tubular epithelium contact) leads to decreased Na+ resorption, resulting in increased natriuresis. The natriuresis is minor in comparison to the osmotic diuresis, so hypernatremia may occur.
Indications
Osmotic diuretics are used when increased water excretion with minimal Na+ excretion is required. For example, it can be indicated to treat conditions associated with impaired renal hemodynamics or to maintain urine volume and prevent anuria, which may occur during hemolysis. Osmotic diuretics can also be prescribed to decrease intracranial or intraocular pressure as they reduce the rate of aqueous humor production. Finally, mannitol can be used along with loop diuretics to induce forced diuresis in intoxication (to decrease the plasma concentration of the toxin).
Contraindications
Osmotic diuretics should be avoided in patients with anuria (since no urine is produced, diuretics will not reach their typical site of action, but they will only affect other organs) or heart failure.
Side effects
- Mannitol is quickly diffusing in the extracellular fluid, which draws out water from the intracellular fluid, resulting in dilution hyponatremia and increased extracellular and intravascular fluid volumes.
- Common side effects include headache, nausea, and vomiting.
- Concurrent heart failure may result in acute pulmonary edema.
- High doses of mannitol without adequate water replacement may result in dehydration and hypernatremia.
Links
Related Articles
Source
- MARTÍNKOVÁ, Jiřina – MIČUDA, Stanislav – CERMANOVÁ, Jolana. Vybrané kapitoly z klinické farmakologie pro bakalářské studium : Kardiovaskulární systém [online]. ©2000. [cit. 2010-07-02]. <https://www.lfhk.cuni.cz/farmakol/predn/bak/kapitoly/prednasky/kardio-bak.ppt/>.
</noinclude>
Aquaretics
Aquaretics are receptor blockers for ADH.
- Vaptans, non-peptide low molecular weight V1 and V2 receptor antagonists:
- conivaptan,
- reabsorption mainly of water,
- treatment i.v. (low BAV),
- indications: hyponatremia due to eg SIADH (Syndrome of Inappropriate ADH).
Links
Related Articles
- Renin-angiotensin-aldosterone system
- Hypertension
- Hypertensive crisis
- Treatment of coronary heart disease
External links
Source
- MARTÍNKOVÁ, Jiřina – MICHUDA, Stanislav. Selected chapters from clinical pharmacology for bachelor study : Cardiovascular system [online]. ©2000. [cit. 2010-07-02]. <https://www.lfhk.cuni.cz/farmakol/predn/bak/kapitoly/prednasky/kardio-bak.ppt/>.
- ŠTĚRBA, Martin. Selected chapters from pharmacology - lectures / seminars : Diuretics [online]. ©2008. [cit. 2010-10-11]. <https://www.lfhk.cuni.cz/farmakol/predn/cz/2008/2008-diuretika_web.ppt/>.