Hypoglycemia
Hypoglycemia is blood glucose level lower than normal, this value varies depending on age and the literature source:
- 3,3 mmol/l[1], in infants and older children below 2.2 mmol/l (whole blood, 10-15% higher when determined from serum or plasma);[1]
- 2,2−2,6 mmol/l in adults and children;[2]
- in newborns 1,7 mmol/l and premature babies 1,1 mmol/l.[3]
When hypoglycaemia is imminent the insulin secretion decreases but the secretion of cortisol, growth hormone, catecholamines and glucagon increases. There is an increased glucose production by glycogenolysis, gluconeogenesis and at the same time, the peripheral utilization of glucose decreases. Severe hypoglycaemia is an acute, life-threatening condition.[1]
Clinical manifestations of hypoglycaemia include:
- signs of catecholamine washout: sweating, palpitations (tachycardia), pallor, paresthesia, tremors, anxiety, weakness, nausea and vomiting;
- sings of brain glycopenia: headache, confusion, somnolence, speech impairment, diplopia, personality changes, inability to concentrate, staring, hunger, convulsions, ataxia, stroke, coma.[4]
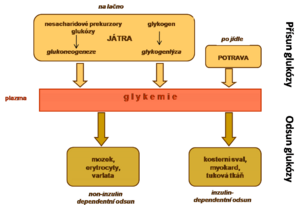
Importance of glucose[edit | edit source]
.Importance of Glucose:
- basic substrate of energy metabolism,
- instant energy source — oxidation of 1 mol of glucose produces 38 mol of ATP,
- source for energy storage in the form of glycogen, fat and protein,
- a key substrate of the brain's energy metabolism — decrease in glucose diffusion to the brain leads to hypoglycorrhagia and energy deficit in neurons, resulting in brain edema, unconsciousness, convulsions and rapid fatal consequences,
- in infants, an additional substrate for the synthesis of membrane lipids and proteins required for brain maturation and myelination.[1]
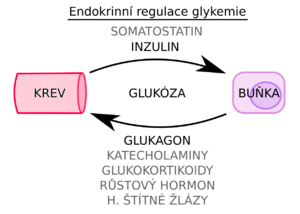
Glycaemic control[edit | edit source]
Normoglycaemia is maintained by a simple feedback loop at the level of pancreatic β-cells. The enzyme glucokinase triggers or inhibits a cascade of intracellular events that lead to the release of insulin from intracellular granules into the bloodstream, depending on the level of glycaemia.
The so-called counterregulatory hormones of glucose homeostasis - glucagon and catecholamines - are also involved in glycaemic control, preventing glucose from falling below the lower limit of the normal range.
In the long term, cortisol and growth hormone are also involved in glycaemic control, increasing insulin resistance, i.e. weakening the effects of insulin.[1]
Etiology[edit | edit source]
| Classification of hypoglycemia in children[4] | ||
|---|---|---|
| Hormonal disorders | Deficiency of counterregulatory hormones | panhypopituitarism, isolated growth hormone deficiency, ACTH deficiency (↓ cortisol), Addison's disease (↓ cortisol), glucagonu deficiency, adrenaline deficiency. |
| Hyperinsulinism | newborn of a diabetic mother, fetal erythroblastosis, childhood persistent hyperinsulinaemic hypoglycaemia, insulinoma, Beckwith-Wiedemann syndrome, antibodies against insulin receptors. | |
| Lack of substrate | Prematurity, low weight for gestational age, ketotic hypoglycaemia, maple syrup disease. | |
| Metabolic disorders | Glycogenolysis disorders | Glycogenosis 0, I, III, VI (ex. Glycogen synthase deficiency, glucose-6-phosphatase deficiency, amylo-1,6-glucosidase deficiency, hepatic phosphorylase deficiency) |
| Disorders of gluconeogenesis | fructose-1,6-diphosphatase deficiency, pyruvate carboxylase deficiency, phosphoenolpyruvate carboxykinase deficiency. | |
| Fatty acid oxidation disorders | LCAD, MCAD, SCAD, Carnitine deficiency, transport disorders of beta-oxidation: carnitine palmitoyltransferase deficiency (CPT I,II). | |
| Other | galactosemia, hereditary fructose intolerance, tyrosinemia propionic acidemia, methylmalonic acidemia, glutaric aciduria; global hepatic dysfunction, Reye's syndrome, hepatitis, heart failure, sepsis, shock, carcinoma/sarcoma, malnutrition, starvation, hyperviscosity syndrome. | |
| Medication/intoxication | hypoglycaemic drugs, insulin, salicylates, propranolol, valproate, pentamidine, quinine, trimethoprim-sulfametaxazole; alcohol]. | |
Types of hypoglycaemia[edit | edit source]
Hypoglycaemias can be divided into two groups according to the causes based on the physiological regulation of glycaemia:
- from insufficient glucose supply to the blood circulation;
- too fast pick-up from circulation.
| A. Reduced glucose supply | B. Increased glucose utilization |
|---|---|
| decreased hepatic gluconeogenesis | increased physical activity |
| inherited metabolic disorders | hyperinsulinism |
| alcohol intoxication | tumour of beta-cells |
| Poisoning | lack of insulin antagonists |
| Malabsorption | M. Addison |
| starvation | hypopituitarism |
| treatment with sulfonylurea | |
| insulin overdose |
However, it is more practical to divide them into the following types.[3]
Hypoglycaemia when fasting[edit | edit source]
They are caused by:
- tumours of β-cells islets of Langerhans (carcinoma, adenoma) or their hyperplasia (nesidioblastosis); extrapancreatic tumours (insulin secreting or non-secreting);
- endocrinopathies causing counter-insulin hormone deficiency (panhypopituitarism, isolated growth hormone or adrenocorticotropin deficiency, hypoadrenalism, hypothyroidism, glucagon deficiency);
- liver cirrhosis' (hepatitis, congestion in the liver in heart failure);
- glycogenoses]' (type I, VII, IX) and defective enzymes of gluconeogenesis metabolism;
- glucose precursor deficiency (alanine) - pregnancy hypoglycaemia, infant ketosis hypoglycaemia, uraemia, severe malnutrition.
Hypoglycemia in newborns and infants[edit | edit source]
In Newborns glucose is lower than in adults (on average 1.94 mmol/l) and shortly after birth it falls further (as the liver glycogen store is depleted) to values of around 1.66 mmol/l in preterm infants and 1.11 mmol/l in term infants, without clinical signs of hypoglycaemia. The most common causes of neonatal hypoglycemia are prematurity, breathing distress syndrome, maternal diabetes mellitus, pregnancy toxemia, hypothermia, polycythemia. Hypoglycemia is usually transient.
In Infants it may no longer be transient and is usually caused by inherited metabolic disorders (galactosemia, glycogenosis, hereditary fructose intolerance, deficiency of gluconeogenesis enzymes) or is ketosis hypoglycaemia, which occurs during fasting or febrile states. Other causes may be leucine hypersensitivity, endogenous hyperinsulinism, Rey syndrome or idiopathic hypoglycaemia (McQuarrie syndrome).
Ketotic hypoglycaemia most often occurs in children between 18 months and 5 years of age. Clinical signs of hypoglycaemia appear after prolonged fasting (often with inappetence during the course of the disease). They are often small, thin children with small energy reserves. This is a per exclusion diagnosis. Treatment consists of an antihypoglycaemic regimen, i.e. a frequent diet high in protein and carbohydrate and prevention of fasting. With dietary refusal, hospitalization for parenteral glucose administration is necessary. It usually resolves spontaneously by 7 to 8 years of age.[4]
Postprandial hypoglycaemia[edit | edit source]
- alimentary (in patients with gastrectomy, gastrojejunostomy, etc..);
- in the early stage of diabetes mellitus;
- functional idiopathic hypoglycaemia;
- leucine-induced hypoglycaemia;
- fructose-induced hypoglycaemia (fructose-1-phosphate-aldolase deficiency or fructose-1, 6-bisphosphate-aldolase deficiency).
Drug-induced hypoglycaemia[edit | edit source]
- insulin;
- oral antidiabetic drugs;
- salicylates, propranolol;
- alcohol (ethanol inhibits gluconeogenesis).
Reactive hypoglycaemia[edit | edit source]
It is a clinical syndrome that manifests itself postprandially (after eating) with signs from the autonomic nervous system (weakness, tremor, cold sweat, nausea, hunger, epigastric discomfort), accompanied by hypoglycaemia (below 2.5-2.77 mmol/l), usually during the day. Reactive hypoglycaemia must be distinguished from hypoglycaemia arising from hunger. Reactive hypoglycaemia is a benign condition and can also be seen as a physiological situation. Glucose determination at the time of onset of clinical symptoms is helpful for diagnosis; a 5-6 hour glucose tolerance test is less appropriate.
„Nonhypoglycaemia“[edit | edit source]
Nonspecific clinical symptoms (fatigue, weakness, palpitations, muscle spasms, dullness, sweating, pain, etc.) that are usually attributed to hypoglycaemia, but have never been proven.
Clinical signs and consequences[edit | edit source]
Clinical manifestations of hypoglycaemia are due to CNS depression from lack of energy substrate and activation of counterregulatory hormones and catecholamine secretion. Symptoms in young children: irritability, feeding problems, pallor, hypotonia, hypothermia, apneic pauses, bradycardia, decreased level of consciousness, convulsions. Symptoms in older children: confusion, irritability, headache, visual disturbances, tremor, pallor, sweating, tachycardia, weakness, convulsions and coma.[4]
Long-term consequences of hypoglycaemia in infancy include mental retardation and secondary epilepsy. Hypoglycaemia also appears to affect personality formation. MRI of the brain shows insufficient gyrification, reduced white matter myelination and atrophy of the cerebral cortex. Even in older children, repeated severe hypoglycaemia can cause permanent neurological and intellectual impairment and secondary epilepsy.[1]
Links[edit | edit source]
Related articles[edit | edit source]
External links[edit | edit source]
- Differenciální diagnostika hypoglykémie prolekare.cz 2020
- Léčba hypoglykémie laiky a zdravotníky prolekare.cz 2019
Reference[edit | edit source]
- ↑ a b c d e f LEBL, J – JANDA, J – POHUNEK, P, et al. Klinická pediatrie. 1. edition. Galén, 2012. 698 pp. pp. 216-217. ISBN 978-80-7262-772-1.
- ↑
- ↑ a b MASOPUST, Jaroslav – PRŮŠA, Richard. Patobiochemie metabolických drah. 2. edition. Univerzita Karlova, 2004. 208 pp.
- ↑ a b c d KLIEGMAN, Robert M. – MARCDANTE, Karen J. – JENSON, Hal B.. Nelson Essentials of Pediatrics. 5. edition. China : Elsevier Saunders, 2006. pp. 785-788. ISBN 978-0-8089-2325-1.
Source[edit | edit source]
- MASOPUST, Jaroslav – PRŮŠA, Richard. Patobiochemie metabolických drah. 2. edition. Univerzita Karlova, 2004. 208 pp.