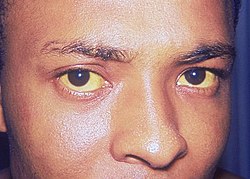
Jaundice
Jaundice[edit | edit source]
Introduction[edit | edit source]
Jaundice, also known as icterus, refers to the yellow discoloration of the skin, sclerae, and mucous membranes caused by an increased concentration of bilirubin in the blood and tissues. Bilirubin is a breakdown product of heme metabolism, and its accumulation reflects a disturbance in any part of the bilirubin pathway, including production, hepatic uptake, conjugation, or excretion. Although jaundice itself is not a disease, it represents an important clinical sign that can indicate a variety of underlying hepatobiliary or hematologic disorders. The evaluation of jaundice therefore relies on understanding bilirubin physiology, classifying the type of jaundice, and identifying the characteristic clinical and laboratory patterns.
Physiology of Bilirubin Metabolism[edit | edit source]
Most bilirubin is formed from the degradation of hemoglobin in senescent red blood cells by macrophages in the spleen, liver, and bone marrow. Heme is first converted to biliverdin and then to unconjugated bilirubin, which is lipid-soluble and must bind to albumin for transport to the liver. Hepatocytes absorb bilirubin and conjugate it with glucuronic acid using UDP-glucuronyltransferase, producing water-soluble conjugated bilirubin. This conjugated bilirubin is excreted into bile canaliculi and delivered to the intestine, where bacterial enzymes convert it to urobilinogen. Part of the urobilinogen is excreted in feces as stercobilin (giving stool its brown color), whereas a small amount is reabsorbed and excreted in urine as urobilin.
Disruption at any point in this system can lead to elevated bilirubin and jaundice, and the pattern of impairment helps identify the underlying cause.
Classification of Jaundice[edit | edit source]
Jaundice is traditionally divided into three categories based on the location of the disturbance: pre-hepatic, hepatic, and post-hepatic jaundice.
Pre-hepatic Jaundice[edit | edit source]
Pre-hepatic jaundice results from excessive production of bilirubin, usually due to accelerated red blood cell destruction. The liver’s conjugating capacity becomes overwhelmed, leading to an isolated increase in unconjugated bilirubin. Conditions such as hemolytic anemias, G6PD deficiency, sickle cell disease, thalassemia, and the resorption of large hematomas commonly produce this form of jaundice. Because conjugated bilirubin remains normal, urine bilirubin is absent, although urobilinogen may be elevated due to increased bilirubin entering the intestine.
Hepatic (Hepatocellular) Jaundice[edit | edit source]
Hepatic jaundice occurs when hepatocytes are unable to efficiently uptake, conjugate, or excrete bilirubin. This leads to a mixed elevation of both unconjugated and conjugated bilirubin. Viral hepatitis, alcoholic hepatitis, drug-induced liver injury, autoimmune hepatitis, cirrhosis, and inherited disorders such as Gilbert syndrome or Crigler-Najjar syndrome represent common causes. The presence of hepatocellular injury disrupts bile canalicular secretion, contributing to cholestasis. Clinically, patients often present with systemic symptoms of liver inflammation such as fatigue, nausea, and right upper quadrant discomfort.
Post-hepatic (Obstructive) Jaundice[edit | edit source]
Post-hepatic or cholestatic jaundice results from obstruction of bile flow after conjugation, leading to a predominant rise in conjugated bilirubin. Gallstones, pancreatic cancer, cholangiocarcinoma, strictures, parasitic infections, and primary sclerosing cholangitis are classic causes. Conjugated bilirubin regurgitates into the bloodstream and is excreted in the urine, causing dark urine. Because stercobilin is absent, stools appear pale or clay colored. Pruritus is particularly characteristic due to retained bile salts.
Pathophysiology[edit | edit source]
The development of jaundice depends on whether bilirubin is unconjugated or conjugated. Unconjugated hyperbilirubinemia reflects either excess production or reduced conjugation. Because it is lipid-soluble, unconjugated bilirubin does not appear in urine and can cross the blood–brain barrier, posing a risk of kernicterus in neonates.
Conjugated hyperbilirubinemia, on the other hand, arises when excretion is impaired; conjugated bilirubin is water-soluble and therefore appears in urine, producing dark discoloration. Cholestasis causes the accumulation of bile acids and contributes to pruritus, malabsorption of fat, and vitamin K deficiency.
Clinical Manifestations[edit | edit source]
Early jaundice is often most visible in the sclerae due to their high elastin content. Patients may complain of dark urine, pale stools, pruritus, fatigue, abdominal discomfort, or symptoms related to the underlying disease, such as fever in cholangitis or arthralgias in viral hepatitis. Chronic cholestasis can lead to deficiencies in fat-soluble vitamins, especially vitamin K, resulting in coagulopathy.
Laboratory Findings[edit | edit source]
The distinction between types of jaundice is strongly supported by biochemical testing:
Pre-hepatic jaundice:
Unconjugated bilirubin is elevated, while conjugated bilirubin and liver enzymes are normal. Markers of hemolysis such as LDH and reticulocyte count are increased, and haptoglobin is low.
Hepatic jaundice:
Both bilirubin fractions are elevated. AST and ALT are typically increased because of hepatocellular injury. ALP and GGT may rise when cholestasis is present. Synthetic dysfunction leads to elevated INR and low albumin in advanced disease.
Post-hepatic jaundice:
Conjugated bilirubin is markedly elevated, along with cholestatic enzymes (ALP and GGT). Pale stools and dark urine are characteristic.
Diagnostic Approach[edit | edit source]
Evaluation begins with determining whether hyperbilirubinemia is conjugated or unconjugated. When unconjugated bilirubin predominates, hemolysis should be investigated. When conjugated bilirubin is elevated, differentiation between intrahepatic disease and extrahepatic obstruction is essential. Liver enzymes help guide this distinction: a hepatocellular pattern (AST/ALT > ALP) suggests hepatic jaundice, whereas a cholestatic pattern (ALP/GGT > AST/ALT) suggests obstruction. Ultrasound is typically the first imaging method to assess biliary dilation, followed by MRCP or ERCP if obstruction is suspected.
Summary[edit | edit source]
Jaundice is a clinical sign caused by elevated bilirubin and reflects disturbances in bilirubin metabolism or biliary excretion. Understanding bilirubin physiology enables differentiation among pre-hepatic, hepatic, and post-hepatic jaundice. Laboratory evaluation and imaging guide diagnosis and management. Recognizing the characteristic patterns of jaundice is essential for identifying life-threatening causes such as biliary obstruction or severe liver disease.
Sources[edit | edit source]
1. Kumar V., Abbas A.K., Aster J.C.
Robbins and Cotran Pathologic Basis of Disease, 10th edition.
Elsevier, Philadelphia, 2021.
2. Hall J.E., Guyton A.C.
Guyton and Hall Textbook of Medical Physiology, 14th edition.
Elsevier, Philadelphia, 2021.
3. McCance K.L., Huether S.E.
Pathophysiology: The Biologic Basis for Disease in Adults and Children, 8th edition.
Elsevier, St. Louis, 2019.
4. AMBOSS Medical Knowledge Platform.
Articles on Jaundice, Liver Failure, and Shock Physiology.
Accessed 2024.
5. UpToDate, Wolters Kluwer.
Articles: “Evaluation of Jaundice in Adults,” “Acute Liver Failure,” “Shock: Definition, Pathophysiology, Types.”
Accessed 2024.