Electrocardiogram manifestations of disturbances of impulse generation and conduction
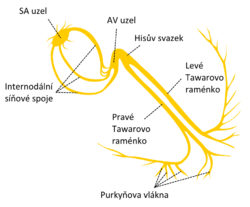
Excitation (depolarization) usually begins in the sinoatrial node. It propagates as a wave through the atrial musculature. It may pass to the ventricles via the atrioventricular node, His bundle, Tawar's arms, and Purkinje fibers. The atria are electrically isolated from the ventricles.
| atrial muscle | 1 m/s |
| His bundle, Tavar's arms, Purkinje fibers | 4 m/s |
| ventricular muscle | 0.5 m/s |
| SA node | 60-100/min |
| AV node | 40-55/min |
| His bundle, Tavar's arms, Purkinje fibers | 25-40/min |
Physiological duration of individual waves, segments and intervals on ECG[edit | edit source]
| wave P | 60-100 ms |
| wave T | 200 months |
| interval PQ | 120-200 ms |
| QRS complex | 60-100 ms |
| QT interval | 340-420 ms |
Disturbances of excitation[edit | edit source]
- Sinus rhythm
Depolarization in the healthy heart begins in the SA node. This is homotopic automation and we refer to the resulting rhythm as sine. On the EKG, each QRS complex is preceded by a P wave.
- Atrial rhythm
Depolarization begins in the atria outside the SA node.
- Nodal (junctional) rhythm
Depolarization occurs in the AV node.
- Vatrial rhythm
Depolarization can also start in the ventricles, then we talk about the so-called "ventricular" rhythm.
- All non-sinus rhythms are arrhythmias.
Faults in SA node[edit | edit source]
The reasons for SA node disturbances are not yet well understood. The influence of ischaemic, hypoxic, acidosis and ion disruption conditions are thought to impair SA node function.
Its damage results in two clinical syndromes:
- sinus arrest
- sick SA node syndrome (sick sinus syndrome).
SA node automatic function interruption (sinus arrest) may manifest as dizziness to syncope due to a failure of cardiac contraction when the interruption lasts longer than 3 seconds. The blackout may be accompanied by the development of excitation in the more distal parts of the transduction system = leaky excitation/rhythm.
The sick sinus syndrome is characterised by paroxysmal or prolonged sinus bradycardia with little acceleration on physical exertion, fatigue and vertigo. A delayed QRS complex appears on ECG. In sick SA node syndrome, bradycardia is often present, interspersed with paroxysms of tachycardia of the nature of supraventricular tachyarrhythmias.
Excitation generation outside the SA node[edit | edit source]
The active source of excitations that lead to depolarization is a site other than the SA node. This occurs when the new excitation source is faster than the SA node's automation. If it is a single excitation, it is a premature contraction - extrasystole (the cause is usually ischemia, myocardial hypoxia, acidosis, etc.). It may also be a faster rhythm that follows a premature contraction - tachyarrhythmia (attributed to the reentry phenomenon or subsequent early or late repolarizations). Both of these disorders may have a supraventricular as well as a ventricular cause.
Supraventricular rhythms[edit | edit source]
Supraventricular Rhythm:
Supraventricular Tachycardia:
The site of their origin is above the ventricles (SA node, atrial musculature or AV node). Depolarizations propagate to the ventricles normally, quite independently of where the supraventricular begins. The QRS complex is uniform, narrow and normally shaped. Repolarization is normal, the T wave is physiological.
ECG curve
- TF'' 60/min;
- axis'' intermediate;
- P'' negative;
- PQ' 0.10 s;
- QRS' 0.09 s;
- ST' mild depression in V5-V6;
- T negative in V5–V6 (Fig).
Nodal Rhythm (Fast - Upper)'
- P negative in almost all leads: retrograde propagation of the impulse from the AV node to the atrium → nodal rhythm.
- Nodal rhythm: 40-60 beats/min → on the upper limit - relatively fast.
→ Both suggest a pacemaker in the upper part of the AV node. (pic.)
Atrial extrasystoles
If they are isolated, they do not affect hemodynamics. The P wave comes earlier after the previous U wave and can be overlapped by it. It can be biphasic or inverted. The PQ interval may be shortened. The QRS complex is normal.
Junctional (AV) extrasystoles
During the period of the ventricular complex, retrograde depolarization of the atria takes place, the P wave is not shown. They do not affect hemodynamics.
Atrial supraventricular tachycardia
The source of the excitation is the reentry phenomenon, the automatic activity of the ectopic site or multiple ectopic sites. It has the character of paroxysmal and non-paroxysmal tachycardia.
Atrioventricular junctional supraventricular tachycardia
It is most often a reentry phenomenon in the area of the AV node. Mostly paroxysmal form with a frequency of 140-180/min. The P wave is absent during the attack.
Atrioventricular reentry supraventricular tachycardia
Nejčastěji jde o reentry fenomén v oblasti AV uzlu. Mostly paroxysmal form with a frequency of 140-180/min. The P wave is absent during the attack.
- Atrioventricular reentry supraventricular tachycardia
Occurs because there is an accessory connection between the atria and ventricles. Conduction may be anterograde (from atria to ventricles) or reversed.
Ventricular rhythms[edit | edit source]
They begin in the ventricles, with depolarization spreading relatively slowly over the ventricular musculature - QRS complexes are wide and abnormally shaped. Nor does repolarization proceed in the usual manner - the T wave is inverted. There may also be ventricular extrasystoles and tachycardia.
- Ventricular extrasystoles
The excitation originates distal to the bifurcation of the bundle of His or in the Purkinje fiber network. The excitation propagates further along accessory pathways, sometimes retrograde, which takes longer than normal depolarization. The QRS is wide and atypical in shape. They may be compensated - one or more of the excitations from the SA node do not apply. The site in the ventricle where the excitation originates may be one or there may be several.
- Ventricular tachycardia
On ECG we see a series of at least three extrasystoles with a frequency above 100 revolutions/minute. We also see a wide QRS complex that is abnormal in shape. The shape of the QRS can be either uniform - monomorphic' or polymorphic'. Hence the monomorphic or polymorphic ventricular tachycardia. It may cause worsening of left-sided heart failure, or be associated with ischaemic pain - inducing a sensation of palpitations, syncope or progressing to ventricular fibrillation. Causes include acute or chronic ICHS, hypertrophic or dilated cardiomyopathy, congenital prolonged QT interval syndrome.
Conduction disorders[edit | edit source]
Conduction slowing[edit | edit source]
Atrioventricular block + bundle branch block[edit | edit source]
Cannot be distinguished from each other from surface ECG alone. The PR interval is the time it takes for depolarization to propagate from the SA node through the atria, AV node, along the bundle of His to the interventricular septum. If the PR is longer or if the QRS complex is absent after the P wave, it is a conduction disturbance. The AV node is a natural retarder of atrial to ventricular conduction. Its function deteriorates most often in IHD.
- Grade I AV block
Grade I AV block means that each atrial depolarization is followed by ventricular depolarization, but AV conduction is slowed (prolonged PR interval). It can occur in healthy people, but can also signal e.g. acute myocardial infarction. Cardiac function does not deteriorate, therefore it remains asymptomatic.
Other signs of grade I AV blockade:
- Prolonged atrial conduction.
- All atrial impulses are transferred to the ventricles.
- PQ = 0.22 s → prolonged AV conduction → grade I AV block.
- The "U" wave is not a U wave, but a P wave.
- The QS in aVR is the normal sinus potential from the right ventricle (Figure 1).
EKG waveform
- TF 84/min;
- sinus rhythm;
- semi-horizontal axis;
- PR in II = 11,5 mm = 0,23 s;
- QRS 0,09 s;
- QS in aVR?!;
- ST in the isoelectric line;
- T wave normal direction. (pic.)
- AV blockage grade II
Grade II AV block occurs when atrial depolarization is transmitted to the ventricles intermittently. There are 2 types:
- Type I (Wenckebach type). The duration of the PQ interval is progressively prolonged with each successive heartbeat to values greater than 0.2 s. Na konci periody se jeden vzruch nepřevede vůbec a tak se znázorní jen vlna P. Pak se nastartuje nový cyklus s PQ intervalem kratším než 0,2 s. Porucha vedení je nejčastěji v AV uzlu.
- Type II (Mobitz type).' Here is the normal length of all PQ intervals. Occasionally, there is no transfer of excitation from the atria to the ventricles. In that case, only the P wave is shown and the pulse wave is also absent in the periphery. The danger of this blockade is the possibility of its sudden worsening, when the transmission through the AV node ceases completely and a grade III AV block develops. This results in a decrease in cardiac output with possible loss of consciousness (Adams-Stokes syndrome). The disorder is most commonly in the bundle of His.
ECG curve
- rhythm sinus rhythm;
- PQ' 0.20 s;
- axis'' intermediate;
- QRS'' 0.08 s;
- P wave'' interferes with T wave;
- Atrial TF'' 86/min;
- TF komor 43/min;
- QRS převede se každý druhý;
- ST horizontální deprese 1,0 mm ve V4–V6;
Conclusion
- Atria and ventricles are not independent → it is not an AV dissociation. PQ intervals are constant → they are not Wenkebach periods.
- AV block II st. constant 2:1 (Mobitz II).
- Repolarization disorders → v. s. ischemia.
- The patient has a pacemaker implanted (picture).
- AV block III. degrees
Caused either by damage to His's bundle or by a two-sided interruption of the wiring in Tawara's arms. If the QRS is narrow, the rhythm originates in the bundle of His. If the QRS is wide, the depolarization originates from the Purkinje fibers. Complete AV block impairs cardiac output. The effect of synchronized contraction of the atria and ventricles is canceled. Cardiac output is reduced due to a slow rate of ventricular contractions.
Tawar arm blocks[edit | edit source]
If conduction in the bundle of His is normal and one of the bundle branches is blocked, the PR interval is normal but the QRS is widened. This occurs as a result of delayed depolarization of the part of the ventricle that is supplied by the blocked arm. The blockage does not impair cardiac performance and is asymptomatic.
ECG curve
- P 0.18 s;
- RR intervals'' regular;
- TF' 84/min;
- axis'' horizontal
- S ve III > S ve II;
- RR' ve V1-V3;
- QRS' 0.19 s;
- Q' present in V1-V3;
- ST' descending depression in V1-V4;
- T' negative in V1-V4 (Fig.).
Conclusion
- QRS distorted but P present → not an idioventricular rhythm.
- "M" shape in the leads from the right precordium → BPTR.
- S in III > S in II → extremely horizontal axis (axis deviation to the left) → anterior hemiblock.
- Pathological Q in V1, V2, V3 → anterior IM of older date.
- Complete BPTR. Front IM of older date. Left anterior hemiblock (Fig).
Right bundle branch block
Characterized by an RSR' image in lead V1.
- Left bundle branch block
Characterized by a negative and wide QRS in leads V1–V4 and a discordant ST segment and T wave. If bundle branch block is associated with first-degree AV block, it is likely that the bundle of His or the remaining bundle branch is also damaged. There is a risk of bilateral bundle branch block and with it complete AV block.
- Left anterior hemiblockade - the left anterior fasciculus is narrower, longer, and exposed to greater pressure in the outflow part of the left ventricle compared to the posterior one. For this reason, it is more vulnerable and more often blocked than the posterior fasciculus.
- Left posterior hemiblock - the posterior bundle is much stronger than the anterior and is supplied by both coronary arteries. Its blockade signals a greater extent of myocardial damage.
Conversion acceleration[edit | edit source]
If there is a change in the direction of depolarization propagation in some part of the heart, a conductive pathway can be formed as the basis for the circular reentry phenomenon. Depolarization circulates along this pathway and causes tachycardia. The anatomical basis for the reentry phenomenon is a conductive path that first branches and then connects again. If one branch of this path is blocked, the excitation can propagate back along the damaged branch away from the connection point. Once the reentry phenomenon occurs, it can continue until one part of the path is unblocked.
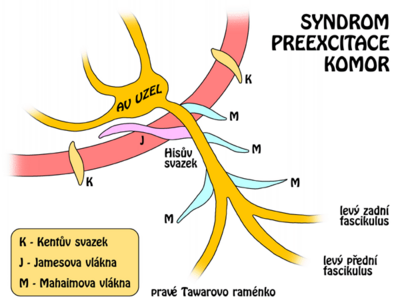
Wolf-Parkinson-White syndrome (WPW syndrome)
WPW syndrome is a classic example of the reentry phenomenon. An accessory conduction pathway is present, either between the right atrium and the ventricle or between the left atrium and the ventricle. In both cases, the AV node is avoided. Physiological ventricular delay is lost, therefore ventricular depolarization begins prematurely. On the EKG we see a shortening of the PR interval and a slowing of the rise of the R wave = delta wave. The depolarization spreads anterogradely along the normal pathway and retrogradely along the accessory pathway, resulting in reactivation of the atria and tachycardia.
ECG waveform:
- rhythm sinusoidal;
- TF 74/min;
- axis (semi)vertical;
- PQ 0.10 s;
- QRS 0.11 s;
- delta wave in almost all leads;
- ST in the isoelectric line;
- T normal direction.
Conclusion
- Preexcitation: Wolf-Parkinson-White syndrome.
- WPW: Bundle of Kent: connection between the atria and the ventricular muscle. Delta wave is present, QRS is prolonged.
- LGL: James's Bond: Link between the Halls and His's Bond. The delta wave is absent, the QRS is not prolonged (Fig.
Sources[edit | edit source]
External sources[edit | edit source]
Used literature[edit | edit source]
- HAMPTON, John R. EKG v praxi. 4. edition. Praha : GRADA Publishing, a.s., 2003. 416 pp. ISBN 80-247-1448-5.
- NEČAS, Emanuel. Patologická fyziologie orgánových systémů I.. 1. edition. Praha : Karolinum, 2006. 380 pp. ISBN 80-246-0615-1.
- ZDENĚK VILIKUS: Přednášky z volitelného předmětu: Interpretace EKG v klidu a při zátěži.