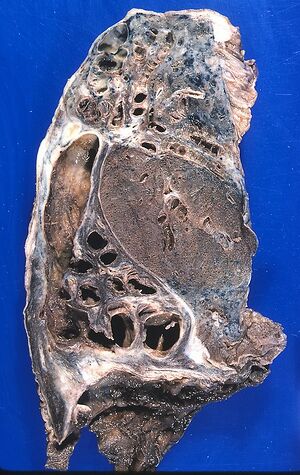
Bronchiectasis (1.LF)
Bronchiectasis is characterised by enlarging of the bronchi, usually followed by their chronic inflammation. It appears most commonly in pre-school and school ages.
Pathogenesis[edit | edit source]
Two important factors play a role: airway obstruction with insufficient mucus drainage and damage to the bronchial wall by infection or aspiration.
- Division by shape:
- cylindrical;
- spindle-shaped;
- varicose;
- sac-shaped.
- Division by etiology:
- idiopathic;
- inborn – on the basis of insufficient cartilage development (Williams-Campbell syndrome), congenital tracheobronchomegaly etc.
- inflammatory – with primary disease such as CF, ciliary dyskinesia syndrome, immune deficits, and others;
- post-infection – with TBC, after measles, pertussis, viral infections;
- post-obstruction – inhaled foreign bodies, external compression of the bronchus, bronchial tumour.
Clinical presentation[edit | edit source]
A typical presentation is chronic cough with sputum production[1], particularly in the morning. During the day the amount of sputum decreases. Auscultation - crackles over the affected area (findings are changeable according to how much the ectases are filled by mucus). Later, chronic hypoxia and cor pulmonale, and clubby fingers develop. In medical history, respiratory infections and dyspnea during exertion are common. The doctor should be alerted to the possibility of bronchiectasis by: chronic cough, lasting atelectasis, unimproving X-ray findings on the lungs after a respiratory infection.
Diagnosis[edit | edit source]
- X-ray of lungs - peribronchial cuffing or areas with atelectases.
- Cystic changes in the lungs are possible.
- Can be assessed well by HRCT; nowadays all non-CF bronchiectases should be diagnosed on the basis of CT examination[2].
- Functional examination - sign of obstruction.
Complications[edit | edit source]
- repeat pneumonia, hemoptysis, cor pulmonale;
- rarely abscesses.
Therapy[edit | edit source]
Therapy consists of infection and bronchial secretion control. The removal of a part of the lung or arterial embolization lower possible complications. Furthermore, positional drainage is used. Mucolytics are used to remove mucus.
Links[edit | edit source]
Related articles[edit | edit source]
Source[edit | edit source]
- BENEŠ, Jiří. Studijní materiály [online]. [cit. 2009]. <http://jirben.wz.cz>.
Reference[edit | edit source]
- ↑ MCSHANE, Pamela J – NAURECKAS, Edward T – TINO, Gregory. Non-cystic fibrosis bronchiectasis. Am J Respir Crit Care Med [online]. 2013, vol. 188, no. 6, p. 647-56, Available from <https://www.ncbi.nlm.nih.gov/pubmed/23898922>. ISSN 1073-449X (print), 1535-4970.
- ↑ HILL, Adam T – PASTEUR, Mark – CORNFORD, Charles. Primary care summary of the British Thoracic Society Guideline on the management of non-cystic fibrosis bronchiectasis. Prim Care Respir J [online]. 2011, vol. 20, no. 2, p. 135-40, Available from <https://www.ncbi.nlm.nih.gov/pubmed/21336465>. ISSN 1471-4418 (print), 1475-1534.