Forum:Seminar papers/Biophysics/2. LF/2018-2019/Group 5/ABE
< Forum:Seminar papers | Biophysics | 2. LF | 2018-2019 | Group 5
Forum:Seminar papers/Biophysics/2. LF/2018-2019/Group 5/ABE
Sonography
Introduction[edit | edit source]
Ultrasound is a medical and diagnostic imaging technique using pulses of high frequency sound waves above 20 kHz. This technique is used to gain advanced insights into the different inner workings of the body based on registration of ultrasound waves reflected from tissues.
Generally there are three different types of ultrasound scans:
- External ultrasound: External ultrasound is used to examine the tissue and organs that can be imaged through the skin. Gel is used between the skin and the probe to ensure that ultrasound is not reflected off the skin but enters the body. This type of ultrasound scan is most commonly used for examination of heart, liver and other organs, as well as a fetus in the womb.
- Internal ultrasound: Internal ultrasound allows a closer look at organs inside the body, such as prostate gland, ovaries or womb by insertion of the probe through anus or vagina.
- Endoscopic ultrasound: In Endoscopic ultrasound technique, an ultrasound probe is inserted into the body usually through mouth to examine areas, such as stomach or oesophagus. The endoscope has a light and ultrasound device at its end. Images are created in the same way as in the external ultrasound method.
Frequencies[edit | edit source]
Ultrasound frequencies in diagnostic radiology range from 2 MHz to approximately 15 MHz: It is important to remember that higher frequencies of ultrasound are absorbed/attenuated more easily (Nadrljansk, 2009). Therefore, higher frequencies are not as penetrating. This explains why high frequencies are used for the superficial body structures and low frequencies are used for those that are deeper.
Medical ultrasound transducers may produce more than one operating frequency. The following frequencies are a guide to frequencies typically used for ultrasound examination:
- 2.5 MHz: deep abdomen, obstetric and gynaecological imaging
- 3.5 MHz: general abdomen, obstetric and gynaecological imaging
- 5.0 MHz: vascular, breast, pelvic imaging
- 7.5 MHz: breast, thyroid
- 10.0 MHz: breast, thyroid, superficial veins, superficial masses, musculoskeletal imaging.
- 15.0 MHz: superficial structures, musculoskeletal imaging.
Modes Of Ultrasound[edit | edit source]
A-mode[edit | edit source]
Display of amplitude spikes of different heights. It consists of X and Y axes, where X represents the depth and Y-the amplitude (Goldberg and Lehmn, 1969). Most commonly used in Ophthalmology for observation of optic nerve. This mode can also be used for echo differentiation of masses as to their cystic or solid nature.
B-mode[edit | edit source]
This is the most common form of ultrasound imaging. It is based on the bright-ness rather than vertical spikes as opposed to the A-mode, hence the name “Brightness modulation”. Brightness refers to the amplitude or intensity of the echo. There are X and Y axes representing depth and lateral position and a grey-scale which represents the intensity of the reflected echo.
M-mode[edit | edit source]
It is also called the “Motion Mode” as it used for examination of moving body parts, most commonly in cardiac and fetal-cardiac imaging. This can be accomplished by recording the depth in real time by repeatedly measuring the distance of the object from the transducer held stationary over the moving tissue.
Doppler-mode[edit | edit source]
Measures velocities of blood in the cardiovascular system.
Acoustic Impedance[edit | edit source]
The physical property of tissues used to describe resistance of tissues to ultrasound waves (Morgan, 2014)
Acoustic impedance relies on:
- density of the tissue (density = kg/m-3)
- Speed of sound in the tissue (v = m/s)
Main formulas are:
- Acoustic impedance is Z = density of tissue * velocity of sound in the tissue
- Reflected fraction R = intensity reflected / incident intensity
The fraction of ultrasound intensity reflected at the interface between two tissues is high when the difference in acoustic impedance of the two tissues is high. Thus materials of similar impedance will not result in much intensity on the display of the machine. But materials that differ significantly in impedance will produce much more “reflected intensity” e.g. Bone has a significantly higher impedance than soft tissue. Resulting in a much higher intensity of reflected sound resulting in a brighter image.
Another significance of this is that when the probe is used on a patient we have to add a gel between the probe and the patients skin, as air has a very low impedance compared to skin and the skin. Therefore if gel is not used the reflection at the skin is almost 100% and no ultrasound enters the body, which means that no image is produced.
Acoustic Impedances of Various Material[edit | edit source]
| Medium | Speed of Sound in Tissue (m/s) | Density of Tissue (kg/m3) |
|---|---|---|
| Air (20oC) | 344 | 1.205 |
| Water (0oC) | 1402 | 1000 |
| Water (20oC) | 1482 | 998 |
| Fat | 1475 | 925 |
| Blood (37oC) | 1570 | 1060 |
| Soft Tissue (37oC) | 1540 | 1060 |
| Brain | 1560 | 1025 |
| Bones | 3360-4080 | 1400-1908 |
| Steel | 5130 | 7874 |
Literature Review[edit | edit source]
Advantages[edit | edit source]
This technique has contributed to diagnosis of different health conditions such as breast lumps, abnormalities in prostate glands, heart diseases, and range of various health complications. However, more importantly, it has a major advantage in observing the prenatal development of the fetus during pregnancy. This non-invasive technique is based on non-ionizing radiation which makes it more advantageous in compare to other imaging techniques based on x-rays.
The main advantage is the fact that it is non-invasive, therefore pretty much reducing the chance of this diagnostic method causing any sort of physical pain or infection. Another useful feature is that the equipment required is portable, and therefore it is extremely accessible even for fragile and sick patients, who may not be able to travel or get about as easily. Ultrasound is also fairly cheap to run and maintain compared to other diagnostic procedures such as CT or MRI. The images provided are real time images and detailed images of soft tissue are better depicted than with radiography. Also more importantly, the use of this procedure is considered to have no side effects on the patient, as they are not subjected to major harmful ionizing radiation.
Limitations[edit | edit source]
- Ultrasound waves are disrupted by air or gas; therefore ultrasound is not an ideal imaging technique for air-filled bowel or organs obscured by the bowel. In most cases, barium exams, CT scanning, and MRI are the methods of choice in such a setting.
- Large patients are more difficult to image by ultrasound because the greater amounts of tissue attenuate (weaken) the sound waves as they pass deeper into the body.
- Ultrasound has difficulty penetrating bone and, therefore, can only see the outer surface of bony structures and not what lies within (except in infants who have more cartilage in their skeletons than older children or adults). For visualizing internal structure of bones or certain joints, other imaging modalities such as MRI are typically used (Kilcoyne et al, 2017)
- Takes a lot of time to do a scan of a wide volume of patient, because it takes some time for the transducer to have proper contact with the skin, be moved in different directions as it scans only a small volume at a time
- Many cancers are not visible on ultrasound
- Sometimes leads to disorder in conductivity of nerve fibers due to the inhibitory effect on the signal propagation
- In elderly individuals, sciatic nerve identification is less successful because of muscle atrophy in which fascia may not be distinguishable
Sonography Images and Patterns[edit | edit source]
Normal Breast Parenchymal Patterns[edit | edit source]
In the young non-lactating breast, the parenchyma is primarily composed of fibroglandular tissue, with little or no subcutaneous fat. With increasing age more and more fat gets deposited in both the subcutaneous and retromammary layers.
Breast Cysts[edit | edit source]
Breast cysts are the commonest cause of breast lumps in women between 35 and 50 years of age. A cyst occurs when fluid accumulates due to obstruction of the extralobular terminal ducts, either due to fibrosis or because of intraductal epithelial proliferation. A cyst is seen on US as a well-defined, round or oval, anechoic structure with a thin wall. They may be solitary or multiple.
Breast Tumours[edit | edit source]
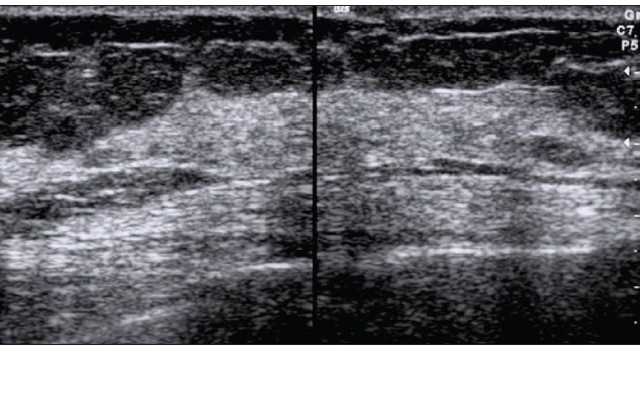
A breast ultrasound is a helpful test in distinguishing between solid and cystic masses. In look-ing at an ultrasound report, the term "hypoechoic" refers to an area on the study that appears darker, and means the area is solid.
Mass Due to Cancer
On ultrasound, a breast cancer tumor is often seen as a solid mass (hypoechoic), that has irregu-lar borders, and may appear spiculated. Other findings on ultrasound that suggest a mass is breast cancer include:
- Non-parallel orientation (not parallel to the skin)
- A mass that is taller than it is wide
- Acoustic shadowing
- Microlobulation
- Duct extension
- A branch pattern
- A mass within a cyst
- Angular margins, which means an irregular or jagged appearance to the mass
Reading the Sonogram[edit | edit source]
The image obtained is mostly a gradient black and white outlines due on the different intensity of the reflected waves The ability of the wave to be reflected to the transducer is called as Echo-genicity.
Hyperechoic Areas[edit | edit source]
The white areas on the screen (more echogenic) due to the greater ability to reflect waves. Usually these areas have high density thereby leads to greater reflection ac-cording to acoustic impedance e.g., bones
Hypoechoic Areas[edit | edit source]
The grey areas on the screen (less echogenic). These areas reflect low in-tensity. In these cases the mass needs to be looked further by MRI or CT scan. It is due to the substance being denser than usual. Hypoechoic masses are mostly found in the liver.
Anechoic Areas[edit | edit source]
The black areas in the image (no echogenicity) it is due to the absence of transmitted sound waves. It mostly includes body cavities or substances with low density.
Practical Tasks[edit | edit source]
Tasks[edit | edit source]
Task 1[edit | edit source]
Register and record image of provided dummy as accurately as possible, sketch the image of structures from different angles and perspectives in the report.
Task 2[edit | edit source]
Identification of individual internal structures within the dummy, measure their size and identify their location within the dummy.
Equipment[edit | edit source]
SonoSite 180 plus portable ultrasound device (“SonoSite”).
Modes:
- 2D (B-scan)
- M-mode
- Doppler Modes.
The imaging device shows the classic “Sector-Shaped” image. The low frequency probe is ideal for sonography aimed at imaging deeper structures and narrower or restricted locations (for ex-ample is cardiology exams) at the cost of lower spatial resolution at closer distances. For this ex-periment we will be focusing on the 2D(B-scan) mode.
Getting Familiar with the SonoSite[edit | edit source]
2D Imaging and measurements:
The default mode is 2D, if it does not default to 2D you can manually do so by pressing the 0 key. By pressing the “patient” button you will be promoted to enter patient specific information, this is important to save your data.
The SonoSite is equipped with a movable screen by gently pulling the screen away from the base it also has options to change the contrast and brightness (using the gain) and field of view. You may need to adjust the gain and/or field of view by pressing the “Depth” key. You may also zoom to 2x magnification by using the “Zoom” key. The “Freeze” key is used to instantaneous freeze an image.
In the 2D method you may extract measurements such as length, area and circumference. These measurement can only take place on a frozen image. By using the “Measure” key, two calipers will appear along with measurement options. Choose your desired option and use the trackball to orientate your measurement and use the “Select” key to implement your desired location. After you have taken all the required measurement you may unfreeze the image to get out of the measurement mode.
Protocols[edit | edit source]
THE IMAGING DEVICE IS STRICTLY TO BE USED ON THE PROVIDED DUMMY SPECIMEN AND NOT ON YOUR COLLEAGUES
- Ensure the specimen is clean and remove all debris with the provided material. Failure to do so will result in inaccurate measurements.
- Apply a small amount of gel onto the 2MHz convex probe.
- Press and hold the SonoSite power button until a beep sounds. (Power button is located on the left side of the SonoSite handle.)
- Begin to ‘massage’ the probe into the specimen to study the internal structures.
- Optional - Save and transfer the images to a computer (Follow the save procedure be-low)
- To turn the SonoSite off you must again press and hold the power button until two con-secutive beeps sound.
In the event the SonoSite enters into sleep mode you must wake the SonoSite up by pressing any key. Sleep is indicated by a blinking battery charge light.
Saving Images to a Computer[edit | edit source]
Begin by connecting the SonoSite to the computer with the provided equipment. Execute the Site Ling Manager Software. The images should automatically be downloaded and can be viewed by accessing the Praktikum Sono found in the Documents folder which is located on the Desktop.
Conclusion:
While most probably equate an ultrasound guided procedure with a common diagnostic exam done during pregnancy, hospitals, clinics and physicians are using ultrasound in many more ways. Ultrasound has proven to be an effective diagnostic tool for a variety of medical conditions, and it has increased in importance during the past fifty years. The importance of ultrasound is increasing. With continuous advances in technology, there’s no doubt there will be even more uses for it in the future. Having the proper equipment on hand is vital to ensure that every patient receives the most accurate diagnosis possible.
Future of Ultrasound[edit | edit source]
As with other computer technology, ultrasound machines will most likely get faster and have more memory for storing data. Transducer probes may get smaller, and more insertable probes will be developed to get better images of internal organs. With the current pattern of development, 3D ultrasound will be more widely used in the future, as rapid and revolutionary innovations are being developed. One exciting new area of research is the use of Virtual Reality technology in the field of ultrasonography that provides doctor with an image which allows them to "see" inside a patient. This allows for minimally invasive, or in some cases, completely non-invasive observations.
References[edit | edit source]
1. Kilcoyne, A., Shenoy-Bhangle, A.S., Roberts, D.J., Sisodia, R.C., Gervais, D.A. and Lee, S.I., 2017. MRI of placenta accreta, placenta increta, and placenta percreta: pearls and pitfalls. American Journal of Roentgenology, 208(1), pp.214-221.
2. Goldberg, B.B. and Lehman, J.S., 1969. Some observations on the practical uses of A-mode ultrasound. American Journal of Roentgenology, 107(1), pp.198-205.
3. MEFANET, síť lékařských fakult ČR a SR. “Ultrasonografie (2. LF UK).” Vzdělávání Sester – WikiSkripta, www.wikiskripta.eu/w/Ultrasonografie_(2._LF_UK).
4. Morgan, Matt A. “Acoustic Impedance | Radiology Reference Article.”, 2014, Radiopaedia.org, radiopaedia.org/articles/acoustic-impedance.
5. Nadrljanski, Mirjan M. “Ultrasound Frequencies | Radiology Reference Article.” Radiopaedia.org, radiopaedia.org/articles/ultrasound-frequencies.
6. “Ultrasound and Acoustic Impedance.” YouTube, YouTube, 18 June 2017, youtu.be/DqG1jMVsQ8g.