Examination of bleeding
Capillary bleeding[edit | edit source]
Rumpel-Leede test[edit | edit source]
The so-called Rumpel-Leede test is used to determine the resistance of blood capillaries . We determine an area of 4 x 4 cm on the palmar side of the forearm, then put on the cuff of the tonometer and apply pressure (about 100 mmHg) for 5 minutes. In 15 minutes, we count the formed petechiae (10 newly formed petechiae should be a maximum).
Examination of platelets[edit | edit source]
Duke's bleeding time[edit | edit source]
We test the function of platelets, the ability to form a platelet plug. An injection is made into the earlobe. Bleeding should normally stop within 2-4 minutes. A standard forearm cut is also sometimes performed ( 2–9 minutes is the norm here ).
The time is prolonged in thrombocytopenia and thrombocytopathy and von Willebrand disease.
Platelet aggregation[edit | edit source]
The rate of platelet aggregation after the addition of the activator is determined photometrically.
Mean platelet volume[edit | edit source]
It is normally in the range of 6–9 fl. Large platelets are found in some thrombocytopathies.
Examination of blood coagulation[edit | edit source]
Blood clotting, or hemocoagulation, is the third stage of stopping bleeding. The first phase is formed first by reflex, later by humoral stimulation of vasoconstriction. In the second phase, there is activation and adhesion of platelets and the formation of a primary (unstable) platelet thrombus. The third phase then includes the activation of the plasma coagulation cascade and the formation of a fibrin network stabilizing the thrombus.
Iron
Indications for examination of blood coagulation[edit | edit source]
- screening examination – before invasive procedures (surgery, biopsy, etc.);
- suspected bleeding or thrombophilic conditions;
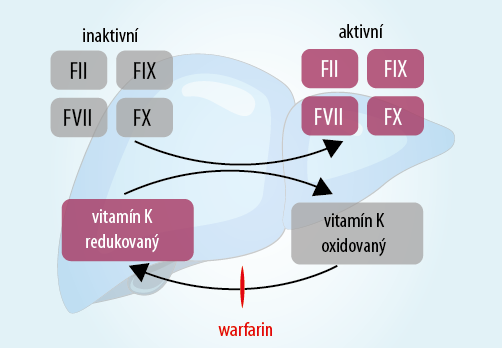
- monitoring of anticoagulant treatment – Warfarin;
- an auxiliary indicator in the evaluation of hepatic proteosynthesis.
Method[edit | edit source]
Blood is collected in a tube with EDTA or with citrate. These substances have the ability to bind calcium (form a complex with it) and thus prevent immediate blood clotting. The blood is sent without delay to the laboratory, where the fraction of blood cells is separated from the decalcified plasma by centrifugation. The required tests are then performed, e.g. aPTT, PT = Quick test, fibrinogen level or D-dimers..
APTT[edit | edit source]
APTT ( activated partial thromboplastin time) is a test of the internal and common pathway of hemocoagulation.
Method[edit | edit source]
At a temperature of 37°C, kaolin - kephalin complex (kephalin - phospholipid from rabbit brain) is added to the decalcified plasma together with an excess of calcium ions. Here, kaolin represents a negatively charged surface that activates the internal pathway, and kephalin functions as a partial thromboplastin (it has nothing to do with tissue thromboplastin!), i.e. actually a substitute for platelet phospholipid, necessary for the activation of factor X. In this way, the internal and then the common pathway is activated. The time until the formation of a fibrin clot is measured.
Physiological values[edit | edit source]
- 25.9–40 s
- APTTR = value for comparison with standard plasma parameter is in the range of 0.83 - 1.3
- APTT is mainly dependent on the initial events of hemocoagulation in the internal pathway (f. XII, XI, IX and VIII), because this part of coagulation takes place more slowly. Only in the second row does it capture the effectiveness of the factors of the common path, X, V, II and I.
Prolongation of APTT[edit | edit source]
- hemophilia A (f. VIII deficiency), hemophilia B (f. IX deficiency), hemophilia C (f. XI deficiency);
- treatment with heparin iv., but not with fractionated heparin sc. - heparin increases the effectiveness of the physiological anticoagulant antithrombin III, which inhibits factors XII, XI, IX, X, II and VII. Except for f. VII, all these changes are included in the APTT. Heparin also directly affects factor X activity;
- Warfarin treatment;
- von Willebrand's disease – a hereditary disorder of vW factor production, which is a carrier of factor VIII and thus affects its activity;
- antiphospholipid syndrome – presence of antibodies against phospholipids;
- consumptive coagulopathy – DIC.
Quick's test[edit | edit source]
Quick's test, PT ( prothrombin time , TT (thromboplastin time)) or thromboplastin time, is a test of the external and common pathway. Indicates the rate of conversion of prothrombin to thrombin due to the action of tissue thromboplastin (coagulation factor III).
Method[edit | edit source]
Tissue thromboplastin is added to the decalcified plasma along with an excess of calcium ions. In this way, the outer and then the common path are activated . The time until the formation of the first fiber of the fibrin clot is measured. The results of the test are usually indicated by the INR index ( international normalized ratio), i.e. the ratio of the patient's measured time and the normal value of the control plasma. Commercially available types of tissue thromboplastin (tissue factor III) differ among themselves. Therefore, the efficiency factor of the thromboplastin used is added to the equation for calculating the INR.
Physiological values[edit | edit source]
- 12–15 p
- INR: 0.8–1.2 (80–120%)
The resulting time depends on the concentration of individual coagulation factors of the external and common system. With increased blood coagulation, the INR is lower, with prolonged coagulation (e.g. during treatment with antivitamin K), the INR increases.
Prolongation of Quick's test[edit | edit source]
- physiologically in newborns – lack of factor VII;
- Warfarin therapy or other conditions with hypovitaminosis K;
- iv. heparin therapy;
- severe hepatic proteosynthesis disorder;
- consumptive coagulopathy – DIC.
Additional examinations[edit | edit source]
- The Lee-White's method
- An indicative method of examining coagulation at the patient's bedside, which has minimal clinical use. The principle of the test consists in the spontaneous activation of the internal coagulation cascade in vitro (in a test tube). The result depends on the state of the internal branch and the common coagulation system.
- Normal time is: 5-15 min at room temperature.
- Total fibrin degradation products
- FDP (fibrin degradation products) and D-dimers are specific for stabilized fibrin (norm below 160 μg/l).
- Immunological determination of fibrin degradation products follows acute phase proteins. It is an indicator of activated fibrinolysis, from a diagnostic point of view, primarily a marker of recently started coagulation with subsequent fibrinolysis. It is mainly used when thromboembolic disease is suspected. However, the high sensitivity of the method comes at the expense of its specificity. It can also be used to monitor treatment in which we are trying to induce clot dissolution in the patient.
- Fibrinogen concentration
- It is referred to as Fbg. This is a determination of the plasma concentration of fibrinogen. The norm is between 1.5-4.5 g/l.
- Antithrombin III
- Assessment of functional activity in plasma, normal range given by comparison with control plasma (70-100%). Primary or secondary (consumption in DIC ) antithrombin III deficiency is a risk factor for thrombophilia .
- Thrombin time
- Thrombin time method (TT, thrombin time ) is a direct examination of the conversion of Fbg to fibrin.
- Method: thrombin is added to the decalcified plasma together with an excess of calcium. The time until the formation of a fibrin clot is measured.
- The physiological range is 17–24 s.
- Prolonged in case of dysfibrinogenemia, severe hypo- or afibrinogenemia, activated fibrinolysis and during treatment with heparin.
- Euglobulin method for determination of fibrinolytic activity
- The euglobulin fraction , containing plasminogen, is precipitated from the plasma at the isoelectric point with acetic acid. The fractions are separated, dissolved and re-precipitated with calcium chloride. The plasmin present, freed from the effect of α2-antiplasmin by precipitation, lyses the formed clot. When the fibrinolytic system is activated, more activated free plasmin is present and clot lysis is faster.
- Physiological lysis time is 120–240 minutes. Shorter times signal increased activation of the fibrinolytic system.
- Activated coagulation time (ACT)
- Blood (which is taken without an anticoagulant) is applied to a test tube with a contact activator (kaolin) and mixed in the device at 37 °C until the coagulation time is read. Routine for checking heparinization in extracorporeal circulation and hemodialysis. ACT of normal blood is approx. 150 s, with heparinization for long-term extracorporeal circulation or hemodialysis 180-300 s, with MO in cardiac surgery > 600 s.
- Another methods of examination
- examination of protein C, protein S, examination of APC resistance (genetically determined resistance of factor V to activated protein C, representing a risk factor for thromboembolic disease);
- examination of antiphospholipid antibodies – lupus anticoagulant, modified aPTT, anticardiolipin antibodies;
- examination of the fibrinolytic system – plasminogen activators (tPA, uPA, PAI-1), plasminogen;
- examination of the activity of individual factors of the coagulation and fibrinolytic cascade - dg. e.g. hemophilia A, B, C.
Evaluation of hemostasis examination[edit | edit source]
| aPTT | PT (Quick) | trombocyty | Doba krvácivosti | Běžné příčiny |
|---|---|---|---|---|
| Vasculopathy, lack of f. XIII | ||||
| ↑ | Trombocytopathy | |||
| ↓ | ↑ | Trombocytopenia | ||
| ↑ | Heparine treatment, lack of f. VIII, IX, XI, XII | |||
| ↑ | Lack of f. VII | |||
| ↑ | ↑ | Warfarinem treatment, another vitamine K hypovitaminoses | ||
| ↑ | ↑ | von Willebrand's disease | ||
| ↑ | ↑ | ↓ | ↑ | Impaired hepatic proteosynthesis, DIC (sepsis) |
loosely based on work by E. Lechler
Links[edit | edit source]
Related Articles[edit | edit source]
External Links[edit | edit source]
Literature[edit | edit source]
Maxdorf. Velký lékařský slovník On-line: Normální laboratorní hodnoty dospělých [online]. ©2008. [cit. 2010-02-28]. <http://lekarske.slovniky.cz/normalni-hodnoty>.